The full article has been originally featured on the Innovation News Network website here and in the 18th edition of their quarterly publication (page 260).
Rather than treat people post-infection, Spectrum Blue is looking to treat surfaces with quantum coatings to prevent infection from taking place.
According to epidemiologists, humanity has entered the post-antibiotic era, in which therapeutic options are fewer and fewer due to the decrease in the number of effective antibiotics.¹ This resistance also extends to disinfectant agents.
Climate change is making conditions for pathogen transmission more prevalent, and rising ambient carbon dioxide correlates with increased viral aerostability and infection risk.
In our homes, mould is linked to allergies and childhood asthma and causes a monumental financial drain on the real estate sector, causing double-digit drops in property resale value.
In the hospital environment, when patients, visitors, or healthcare workers touch contaminated surfaces, they can transmit the microbes to another person or themselves. In the healthcare environment, many assume surfaces that look clean are safe, yet this is not always the case.
Protective strategies
Protective strategies can involve a combination of preventive measures, such as wearing masks or not touching surfaces and, more importantly, cleaning and decontamination methods.
When disinfecting a surface or decontaminating a facility, the efficacy of a disinfectant product is measured by its log reduction, also commonly known as log kills.
The term comes from the logarithm scale, which is used to indicate the percentage of dead bacteria. The term ‘log reduction’ indicates a ten-fold reduction, which means that with every step, the number of bacteria present is reduced by 90%.
Of course, the log reduction is only effective during the contact time of the cleaning agent with the surface containing the bacteria. Once the active ingredient in the cleaning agent has evaporated or been rinsed, the bacteria can return to multiplying.
Bacteria can control and overcome the effect of disinfectants in different ways, such as restricted permeability of the cell wall, the expression of efflux systems, enzymatic degradation, changes in target sites, and the formation of biofilms.²
Unfortunately, as previously mentioned, bacteria also have a tremendous ability to respond to chemical stress caused by biocides, where overuse and improper use of disinfectants can be reflected in a reduced susceptibility of micro-organisms.
Hence, the log reduction is reduced, leading to the need to increase contact time for effectiveness. This poses an issue when using non-persistent cleaning agents as many repeat applications become necessary, increasing personnel exposure to chemicals3 as well as raising operational costs.
All this means that the ideal solution would have to be persistent and would continue the log reduction indefinitely, impeding biofilm formation.
Prevention through coating surfaces
Surface contact is a huge source of contamination and the spread of infections. We share our bacteria and viruses by touching doorknobs, TV controls, tables, chairs, beds, etc.
The microclimate of the medical area provides the bacteria with the survival environment, and the surfaces of the medical habitat provide the material support on which the bacteria will survive.⁴

Biofilm formation constitutes an alternative lifestyle in which micro-organisms adopt a multicellular behaviour that facilitates and prolongs survival in diverse environmental niches. Biofilms form on biotic and abiotic surfaces both in the environment and in the healthcare setting. In hospital wards, the formation of biofilms on walls, ceilings, vents, and medical equipment enables pathogens to persist as reservoirs that can readily spread to patients.⁵
Surfaces such as tall walls or ceilings⁶ , usually more difficult to access and clean, are ideal locations for biofilm formation7 and pathogen shedding. Airborne micro-particles and dust also frequently accumulate on the ceiling, and in damp locations where there is condensation, water droplets (containing bacteria) are formed and fall on work surfaces.
The convection flow caused by our body heat8 or other appliances plays a fundamental role in contaminating the air and surfaces, and transporting pathogens through the hospital environment, especially the ceilings.
Thus, transforming walls and ceilings into persistent cleaning agents would not only stop the formation of biofilm but also decrease the active pathogen load in the air.
This approach has been taken with the development of loaded antimicrobial coatings, such as paints that release silver or copper ions, various biocides and fungicides, or photocatalytic coatings that, when exposed to ultraviolet light, generate free radicals that have an antimicrobial effect.
The first group of coatings, those that release various biocidal agents, has two significant issues. First, they can become depleted and react with many cleaning agents. Second, the substances they release also impact the health of patients and healthcare staff.
The second group of coatings, those that have a photocatalytic effect, had one major issue: They needed UV light, a rare and generally unwanted type of light spectrum inside buildings.
This is where technology has evolved the development of compounds that have electrochemical and photocatalytic effects in visible light as well as in the dark. This is where quantum coatings like the Q-field pigment are needed.
Q-field: What are quantum coatings?
Q-field is a family of patented pigments that use quantum effects to enable coatings to become a persistent log reduction agent without depleting from the substrate, without entering the bacteria, virus, or, most importantly, human beings.
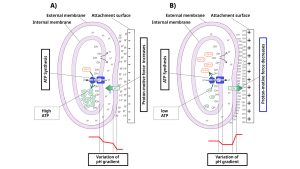
At a quantum level, Q-field microparticles are stimulated by ambient electromagnetic waves to generate surface plasmons and give surfaces a positive charge.
Source: R. Bucuresteanu
With Q-field, the wall or ceiling receives a microscopic force field that deactivates pathogens and stops biofilm and mould from growing.
Once in contact with ambient moisture, this positive charge creates a layer of OH groups that hug the surface of the coated materials. These OH groups hydrolyse the protein structures of viruses, rendering them harmless.
When bacteria attempts surface attachment, the first step in biofilm formation, its electrostatic-sensitive membrane gets broken, and its metabolism is stopped by the OH groups. This is a mechanism that bacteria cannot grow resistant to.
Can we succeed in making safe spaces in our society?
According to the World Health Organization, most countries in the world have not implemented an Infection Prevention and Control programme or an operational plan.⁹ In 2022, only four (3.8%) of the 106 participating countries met all the minimum requirements for Infection Prevention and Control.
Quantum coatings are not poisonous and have a long-lasting effect — a significant improvement in the built environment, materials, and equipment.
If a critical area of surfaces in public buildings, hospitals, nursing homes, elderly homes, restaurants, and hotels were coated, we would have better protection against epidemics and infections.
To have safer spaces, we must also manage all the places that are coated or protected and when such areas should be maintained.
Parallel to this, data on where and how epidemics migrate geographically should be analysed so that we learn more about which public areas should be made safe.
This is why the inventors of Q-field, Spectrum Blue, also introduced an information system (software) to document, manage and map safe spaces in society. This system is designed to support healthcare providers in collaborating and improving infection prevention and control, digitising pathogen surveillance, enabling them to monitor, audit and receive feedback, improve guidelines, and provide education and training to staff.
References
- MDPI | Origin of Antibiotics and Antibiotic Resistance, and Their Impacts on Drug Development: A Narrative Review
- NCBI | Reduced Susceptibility and Increased Resistance of Bacteria against Disinfectants: A Systematic Review
- Oxford Academic | An Overview of Cleaning Agents’ Health Hazards and Occupational Injuries and Diseases Attributed to Them in Sweden
- NCBI | Mechanisms and Impact of Biofilms and Targeting of Biofilms Using Bioactive Compounds—A Review
- NCBI | Bacterial Biofilms: Development, Dispersal, and Therapeutic Strategies in the Dawn of the Postantibiotic Era
- EurekAlert! | Pathogens, including multi-drug resistant “superbugs”, found on floors, ceilings and door handles of hospital toilets, UK study finds
- Toilet microbiome
- Taylor and Francis Online | Experimental and numerical study on the thermal plumes of a standing and lying human in an operating room
- WHO | Global report on infection prevention and control